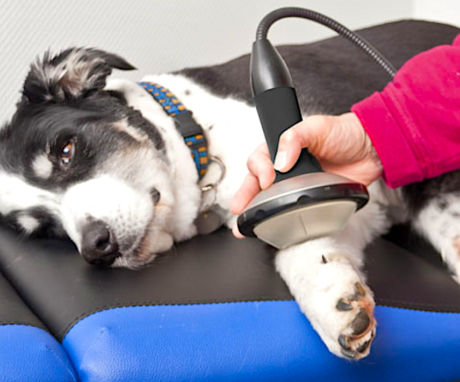
This non-invasive modality can successfully treat a range of orthopedic and soft tissue problems in animals. Though most commonly used for horses, shockwave therapy also has many applications in small animal practice.
Shockwave therapy is a non-invasive treatment that can speed the healing of many types of orthopedic and soft tissue injuries and conditions. It has been used in Europe in human medicine to treat tennis elbow, plantar fasciitis, rotator cuff injuries, calcifying tendonitis of the shoulder, femoral head necrosis, non-union fractures, wounds, burns, osteomyelitis with draining tracts, myofascial pain and more. New research has shown potential applications in treating periodontal disease, infected wounds, and to help speed fracture healing and reduce the incidence of non-union fractures.
In the United States, shockwave therapy has been successfully used for many years in veterinary medicine to treat animals with both acute and chronic soft tissue injuries, bone and joint disease, and back pain. It is also used to aid in wound healing, with and without infection, and to stimulate bone healing, particularly in the case of non-union fracture cases.
Shockwave therapy is widely accepted in equine practice and is commonly used to treat many orthopedic conditions, both bony and soft tissue. While its use is less common in small animal practice, the applications are still numerous. One key to success is an accurate diagnosis and a clearly defined area of injury so you can direct the shockwave to the appropriate area.
Shockwave use in equine practice
In my practice, shockwave therapy is most often used for suspensory ligament injuries, even with avulsion fractures. It can be used on its own for acute injuries or in conjunction with stem cell therapy, PRP injections, or IRAP. It can also be very effective in managing chronic suspensory inflammation of either the body or the branches of the suspensory ligament. It can be a key component in the therapy and rehabilitation of hind limb suspensory ligament injuries, which present a challenging diagnosis at best. In addition to the initial series of treatments in the case of an acute injury, I will also often periodically use shockwave therapy as the horse comes back into work, in an effort to continue to help stimulate healing and remodeling of the injured area.
Good response is also seen in horses with sore backs, including those with muscular pain and pain related to kissing spines. It may be used on its own or in combination with other therapies such as corticosteroid injection of the back musculature, or of the interspinous spaces in the case of kissing spines. I also frequently use shockwave therapy to treat horses with neck pain, including in the upper cervical region and at the poll. I often combine shockwave therapy with chiropractic care in horses with neck, poll or back pain; I find that this combination of therapies can be very effective in managing and relieving pain in these areas.
Other uses include:
- Tendon tears and strains
- Osteoarthritis
- Collateral ligament injuries
- Navicular syndrome
• Ringbone
• Joint inflammation and pain
• Neck pain - Muscle tears and strains
- Infected or large wounds
- Burns
Treatment protocol in equines

The precise treatment protocol depends on the diagnosis of each individual patient. Treatment varies in the number of shockwaves administered and the energy of those shockwaves. Most acute soft tissue injuries are treated a total of three times spaced at two to three week intervals. I typically recommend a re-check exam at three to four weeks after the third treatment to assess the healing that has taken place. In some cases, additional treatments are needed. If shockwave therapy is being used in conjunction with a regenerative therapy such as stem cell or PRP, I would ideally complete one shockwave treatment prior to the regenerative therapy and then would do the second shockwave at three to four weeks after the regenerative treatment, then the third shockwave three weeks after the second treatment.
In cases of osteoarthritis, the protocol is similar, depending on the severity of the degenerative changes. Typically, I would recommend a series of three treatments, spaced at three-week intervals. However, if I don’t see at least a modest improvement by three weeks after the second treatment, I would not do a third. In cases of osteoarthritis that respond well to shockwave therapy, I frequently find it useful to do single “booster” treatments at intervals ranging from three to six months, depending on the individual, his or her workload, and overall response to treatment. In some cases of ringbone, I have had a response lasting up to two years from the initial series alone, and have then come back and done a second series of three, also with positive results. More commonly, I recommend re-treating the horse at a shorter interval in an effort to stay ahead of any decline in comfort. In cases of navicular disease, I also typically recommend a series of three treatments done at shoeing intervals (the frog needs to be pared down and the foot soaked overnight prior to treatment), with “booster” treatments done at three to six month intervals.
The treatments are easily performed at the horse’s home barn, typically with the horse under mild sedation. Sedation may not be necessary, such as when shockwaving the back, neck, or chronic suspensory branches. In cases of acute or recent injuries, sedation is almost always required.
Typically, the horse will start to experience some reduction in pain and/or swelling within hours. This relief will generally last two to four days, then the horse will return to almost his original status. Over the next two to three weeks, however, actual healing will take place. The early response or improvement in comfort is seen both in horses with recent injuries and those with more chronic problems.
Major medical insurance policies for equines will reimburse owners for the cost of focused shockwave therapy. Each policy differs in the coverage offered.
Equine case report
Mary was an 18-year-old Welsh Cob mare used in competitive trail riding (mountainous terrain). She had ringbone RF and was approximately +2 of 5 lame, despite treatment involving corrective shoeing and NSAID therapy. I treated Mary with a series of three shockwave therapy sessions and she was able to return to her previous level of performance for a period of two years, with only intermittent NSAID use. Two years after her initial shockwave therapy series, I did a second series of three treatments and Mary was able to continue competing for one additional year. At that point, the owner opted to retire her. Ringbone is a particularly challenging diagnosis, with limited therapeutic options, so an additional three years of competing thrilled Mary’s owner.
Shockwave use in small animal practice
Shockwave therapy has been successfully used to treat many soft tissue and bony problems, both acute and chronic, in small animals. These include, but are not limited to:
- Hip dysplasia
- Non-union fractures
- Degenerative joint disease
- Spondylosis
- Lumbosacral pain
- Osteoarthritis
- Tendon and ligament injuries
- Bursitis
- Muscle tears and strains
- Wounds
- Lick granulomas
Treatment protocol in small animals
As with horses, the precise treatment protocol depends on the diagnosis of each individual patient. I work with several small animal practices in my area and have helped educate the clinicians about cases that may benefit from a referral for shockwave therapy. If, after learning the details of the case, I think it may be useful, I will then speak with the pet’s owner by phone to discuss the therapy and the expected results, as well as protocol and cost. Some pet insurance companies will cover shockwave therapy for small animals; this is frequently a determining factor in whether or not the owner will opt for it.
If the owner decides to proceed with shockwave therapy, I schedule an appointment at their regular veterinarian’s clinic, and request that the pet come prepared for anesthesia (eight-hour fast). I will then examine the animal and finalize discussions with the owner. We proceed with anesthesia and the treatment is carried out. For follow-up, I request that the owner keep the pet quiet, with leash walks only, for three days after the treatment, then gradually (over a week) return to a normal level of activity. I typically will re-check at ten days and three weeks. At the three-week visit, I again ask that the pet come in fasted and prepped for anesthesia. If, at the three-week exam, the pet has achieved an excellent result, I will opt not to do an additional treatment. If the pet has not achieved the desired improvement, then I will do a second treatment with the same follow-up schedule. It is rare that I would do more than two treatments. The results are typically quite long-lasting, with a range of six to 18 months of pain relief in most cases. As with horses, some pets/cases will benefit from a schedule of “booster” treatments at six-month intervals.
Multiple areas can be treated at one time. As with equines, many pets almost immediately experience a remarkable reduction in pain. Typically, the animal will start feeling a reduction of pain and/or swelling within hours. This will generally last two to four days before the animal returns to nearly the original status. Then, over the next two to three weeks, actual healing takes place.
Small animal case report
Ginger was a 12-year-old mixed breed spayed female dog, weighing approximately 40 pounds, that I saw on a monthly basis for chiropractic care. She had severe degenerative joint disease in both hips and became increasingly uncomfortable. I had discussed shockwave therapy for Ginger’s hips with the owners on multiple occasions, and when Ginger presented +4 of 5 lame on the RH, they finally approved it. On the day Ginger was brought in for shockwave therapy, she was non-weight bearing on her RH. I had some reservation about proceeding with the treatment, but felt that any improvement in comfort would be a success. When Ginger was discharged several hours after waking up from the anesthesia, she was able to walk out of the clinic. At the ten-day re-check, she was bearing 50% weight on her RH, and at the three week re-check, she was bearing 75% of normal weight. I did a second shockwave treatment, and at the three-week check after that, Ginger was bearing 85% to 90% of her full weight on her RH. This improvement in comfort is not attainable with conventional medications. Ginger passed away several months later due to unrelated causes, but remained comfortable on her RH until the end. This case demonstrates the rather dramatic improvement that can be achieved with shockwave therapy.
Selecting your shockwave machine
In this article, I have focused on shockwave therapy, rather than radial shockwave. The physics of the radial wave are completely different. Equine major medical insurance coverage typically will cover only focused shockwave therapy.
Some focused shockwave machines on the market advertise a deeper penetration of the shockwave into the tissue. Considerations here include whether the focal point for the release of the shockwave is so concentrated that there is potential for tissue damage, or a greater likelihood of missing the desired target tissue or injury.
Mechanism of action
A shockwave is a pressure wave – it displaces its surrounding medium. The ripple created when a stone is thrown into a pond is a shockwave. Shockwaves used in veterinary medicine are generated in a fluid medium inside a transducer head, and are then transmitted readily through skin, fat and muscle. The high-energy waves are focused within the transducer head so that the shockwave can be directed to the precise area of an injury. When shockwaves hit an area of higher acoustic impedance, such as bone, they slow dramatically and a large amount of energy is released into the surrounding tissue. Shockwaves are modified or focused for medical/veterinary use so that their energy is released at a specific distance from the point of origin.
Typical characteristics of a shockwave include a short rise time; within nanoseconds, the wave reaches a peak pressure of up to 1,000 times atmospheric pressure. This is followed by a longer period of decreasing pressure, and a return to negative pressure – 10% of the maximum positive pressure – the hallmark of a true shockwave.*
Summary
Shockwave therapy is well-accepted in equine practice as a treatment modality for soft tissue injuries, as well as for a variety of degenerative bony conditions, and neck and back pain. In small animal medicine, there are many indications for which shockwave therapy is very effective, but there is some resistance to it due to the fairly standard requirement for general anesthesia.
Shockwave therapy is an excellent option for animals that can’t tolerate daily anti-inflammatory medication, or are difficult to treat on a daily basis.
My practice is currently comprised of approximately 40% shockwave therapy and 60% chiropractic work, and is approximately 85% equine overall. As a veterinarian who does not compete with local colleagues in the traditional care market, I have been able to develop a very effective working relationship with the other veterinarians in my area. The shockwave portion of my practice originally began solely on a referral basis from other veterinarians. As I have become known in my area for both shockwave therapy and chiropractic care, my shockwave caseload is made up of a mixture of cases referred to me by other veterinarians; cases in which the owner or trainer contacts me directly; and cases that I identify while doing chiropractic work that I feel may benefit from shockwave therapy. In each case, I make a substantial effort to keep the owner’s regular veterinarian “in the loop” about the shockwave therapy I have done, as well as any findings I think may benefit from his/her attention. In that way, I help the animal, the owner and the veterinarian by being an “extra set of eyes” on the patient. Through this consistent effort and respect for practice boundaries, I have been able to establish an excellent working relationship with the other veterinarians in my area.
Shockwave therapy is one of the most exciting therapies to become available to veterinary medicine in quite some time.
Author: Jenny Johnson
Link: https://ivcjournal.com/shockwave-therapy/
*McClure and Dorfmuller. Clinical Techniques in Equine Practice, Dec, 2003.


